Peripheral/Diabetic Neuropathy Treatment, Symptoms, Causes & More

Neuropathy – Polyneuropathy
Neuropathy is term that describes a damage of the nerves. Most common symptoms include: pain (often worse at night), numbness, tingling, ‘pins and needles’, burning sensation, muscle weakness and others. The damage can be caused by different conditions such as disease, infection, injury, medications, toxins or another reason.
Types of neuropathy
• Peripheral neuropathy affects nerves in outer (peripheral) parts of the body such as the feet, legs, hands and arms.
• Proximal neuropathy affects the muscles of the hips and the shoulders.
• Focal or mononeuropathy affects only one nerve. An example is carpal tunnelsyndrome.
• Polyneuropathy affects several nerves. Most people with neuropathy have polyneuropathy.
• Autonomic neuropathy: Nerves of the autonomic nervous system are damaged leading to symptoms such as problems with digestion, blood pressure and bladder function.
• Diabetic neuropathy is caused by diabetes most commonly affects the nerves of of the hands and the feet. It can also affect nerves controlling automatic functions of the body, such as digestion, or nerves in the hips and thighs.
In the UAE Diabetic Polyneuropathy is the most common type. Therefore, we will describe this type below more extensively.
Diabetic Neuropathy
60-70% of people with diabetes are suffering from Diabetic Neuropathies. Neuropathy may be present even before diagnosing diabetes. Diabetes is the most common cause of peripheral neuropathy in the world. However, the symptoms of neuropathy are mostly unknown to the patients and difficult to diagnose. Early diagnosis is important as diabeticneuropathy can damage any nerve in the human body. Be it the nerves controlling the heart beat or the nerves of the skin. Diabetic skin lesions are the major cause of foot amputation.
Causes
Similar to the variety of symptoms there is also a large variety of causes for this disease. The most frequent reason is a metabolic disorder such as diabetes mellitus. But also hereditary disposition, toxic inhibition or paraneoplastic development can cause polyneuropathy.
Signs & Symptoms
Diabetic Neuropathy means the affection of many nerves due to very different reasons and it can therefore develop many different symptoms. Most frequent are paraesthesia such as prickling, numbness, burning of the feet, but also palsies, disorders of speech and failure of cerebral nerves.
Types of Diabetic Neuropathy
There are different types of neuropathy with different typical patterns of pain distribution. For instance there is the:
Symmetric type of diabetic neuropathy
Characterized typically by sensory loss, weakness and painful burning of toes and feet. First symptoms of the symmetric polyneuropathy may appear in the sole of one foot or even involving half a toe, then gradually spreading circumferentially up both legs to the knees, then into thighs and finally the hands. The latter pattern is also termed as “stocking-glove” distribution. Neuropathy always is length-dependent, because the longest axons are the most vulnerable. Patients describe tingling, prickling, burning, numbness and a band like pressure.
Due to sensory deficits, small cuts and wounds will not be noticed by the patients at first thus causing seemingly inexplicable infections. Later, weakness of the muscles will develop, particularly expressed by the fact that patients cannot stand on their heels. With progressing sensory disturbances spreading up also into the tips of the fingers, patients will have difficulties holding objects. Most common is a painful burning in the feet which gets worse with high temperatures. Light stimuli applied to the numb areas may be experienced as extremely painful. Also an imbalance of the gait, getting worse in the dark, is a common symptom of patients with Diabetes.
When the onset of diabetes occurs at a juvenile age of the patients, neuropathies may be first noticed as late as in their thirties to fifties but when the onset takes place at an age over 50, they tend to occur readily with adult-onset. There is a known correlation between the occurrence of neuropathy, the duration and the severity of diabetes, body weight, body size and long-standing hyperglycaemia which must be investigated individually with each patient.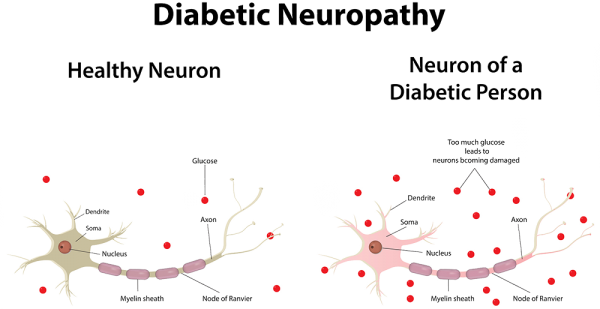
Apart from the above described symmetric form of neuropathy there are other diabetes related neuropathies in different classifications:
Asymmetric diabetic neuropathy
showing focal weakness or sensory loss of single nerves, mainly in one upper arm, one thigh or the cranial nerves.
Asymmetric focal and multifocal types of diabetic neuropathy
of neuropathy are less common, but quite dramatic. They are usually acute in the onset with strong muscle weakness and pain in a thigh or upper arm, but this form rarely occurs before the age of 45. The affection of the cranial nerves causes weakness of the eye muscles accompanied by double images or facial numbness and nerve paralysis.
Autonomic dysfunctions in diabetic neuropathy
Many patients with Diabetes also develop dysfunctions of the autonomic nervous system: constipation, diarrhoea (particularly during the night,), abnormal sweating, hypertension, Tachy- and Bradycardia, dysfunction of the bladder and sexual impotence in males. Symptoms are also uncertain gait, imbalance, maybe syncope’s and blurred vision from lack of papillary regulation.
The distinction between the different kinds of diabetic neuropathy is crucial as far as the different approaches to diagnosis and management are concerned, but also regarding the prognosis.
Treatment
Accordingly, diagnostics and therapy of polyneuropathies are manifold and difficult. The therapeutic aim must be to prevent the deterioration of the nerves itself on the one hand and to treat the illnesses causing polyneuropathy on the other hand. The most essential parts of the evaluation of diagnosis and therapy are…
The most essential part of the evaluation of diagnosis and therapy are – apart from an intensive neurological examination – the electro diagnostic studies of the nerves. The examination comprises Electromyography (EMG) and nerve conduction velocity (NCV). The EMG involves recording electrical potentials by an electrode placed into the muscle, both at rest and during voluntary contractions. The NCV is carried out by stimulating the motor and/or sensory nerves electrically. From the data recorded, informative characteristics of the recorded forms of waves can be determined, thus leading to a clear picture and appropriate treatment.
In the long-term, by way of Diabetes and Complications Control, trial patients who controlled their diabetes meticulously showed significantly less neuropathy. When symptoms of neuropathy occur in patients suffering from diabetes or early signs of polyneuropathic painpatterns as described above, occur, an early neurological examination is of the essence.
Moreover, specialized neuropathic pain treatment can easy the symptoms. Common pain killers are usually not effective enough and anticonvulsants, antidepressants and other drugs need to be used.
Our Team Of Experts
Since more than ten years GNC is the leading clinic for Neurology in the UAE. All our Neuropathy experts are German Board Certified and have minimum professional experience of 25 years. If you are searching for the most trusted Neuropathy experts, you came to the right place.
99% of patients would recommend this clinic. See the full patient satisfaction survey here…
Testimonials
``The doctor is the best and everyone's very helpful``
``Excellent doctor``
``I am thankful for the service.``
``Being able to have blood tests and EEG done at the clinic itself was very helpful and convenient. This also allowed my doctor to have fast access to the test results.``
``I'm impressed by the Professor and team professionalism``
``God bless you guys wish you more of success``
``Great service``
``It was a great visit thanks! It really helped me.``
As Seen On



